

Keeping Orthopaedics Connected in COVID-19.
COVID-19 has caused a major disruption to global healthcare, forcing hospitals to redistribute their resources in response to the pandemic.
This has caused millions of elective surgeries to be cancelled or postponed, with patients awaiting orthopaedic surgeries one of the main groups affected. This has created a backlog of orthopaedic cases, with longer waiting times impacting patient care and wellbeing.
In healthcare, the priority has remained to limit the spread of COVID-19.
This means that orthopaedics has had to lean on innovative technology to keep surgeons, physicians and patients connected. The technology has facilitated diagnosis and care for patients remotely (or with minimal risk of infection), while also helping continue industry processes like training.
Providing Diagnosis for Patients
Working at the point-of-care (POC) does require contact with patients. However, technologies that provide POC diagnostics at doctors’ practices are still crucial to help diagnose and care for patients, while limiting risks of infection. That’s because they keep patients away from hospitals, helping reduce the strains on hospital resources.
US-based Trice Medical are one innovative company providing this solution. Their mi-ultra and mi-eye diagnostic imaging devices help physicians perform full diagnostic arthroscopies and identify joint injuries.
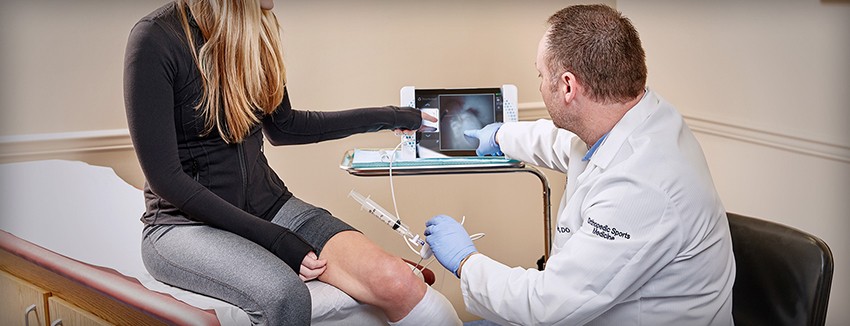 Both devices are handheld and camera-enabled, meaning that they work effectively at POC and help deliver more immediate and definitive patient care.
Both devices are handheld and camera-enabled, meaning that they work effectively at POC and help deliver more immediate and definitive patient care.
Even before COVID-19, Trice Medical were determined to provide an alternative in orthopaedics diagnostics to traditional MRI. Their solutions, like the mi-eye 2, are ready to move this procedure to an in-office setting. This brings advantages including accessibility and a reduced strain on hospital resources.
Caring for Patient’s After Treatment
COVID-19 has also shone a spotlight on remote patient monitoring (RPM) technologies, which are used to support patients after their operations.
The main advantage of this technology during the pandemic is that patients don’t need to come into contact with their physician. That’s because patient data is collected remotely and received by the physician or surgeon via their computer or smart device.
While at the moment the patient benefits include a reduced risk of infection from COVID-19, the long-lasting value to global healthcare goes beyond the pandemic. The reduced face-to-face visits improve productivity and reduce the cost of care, which is important for a health system that continues to be shaped by value.
 California-based Tracpatch provide RPM technology that is focused on post-surgery.
California-based Tracpatch provide RPM technology that is focused on post-surgery.
Their wearable device captures the patient’s daily range of motion post-surgery, monitors ambulation to see movement in action, provides real time feedback on the patient’s exercise compliance and delivers actionable insights on how to aid recovery.
This allows physicians and surgeons to improve patient care pre, intra and post operatively from a remote location. Again, this limits face-to-face visits and saves hospital resources.
Myrecovery.ai are supporting surgeons in a similar way through their artificial intelligence (AI) led App.
Their App allows surgeons to tailor recovery programs for their patients and track progress as they recover. It also hosts real time interactions between patients and surgeons during the treatment pathway. This helps patients gain a better understanding of how to best to take care of themselves.
To support physicians, the App also provides accurate advice throughout recovery based on anatomical data.
Both Tracpath and Myrecovery.ai’s technologies are helping support patient care, which has been challenging during COVID-19 and is especially important for anyone who’s recovering from total joint surgery. This can be very discomforting.
Providing Safe Training & Education
While patient care is the priority, it’s also crucial that processes like training, education and product demonstrations continue throughout the pandemic. That’s why innovative virtual reality (VR) solutions have to come to the forefront to continue these processes throughout COVID-19.
Even before the pandemic, these technologies brought advantages like deeper learning and skill acquisition, improved accessibility and cost-effectiveness. With a stronger reliance on these solutions during COVID-19, more healthcare organisations have become aware of the benefits.
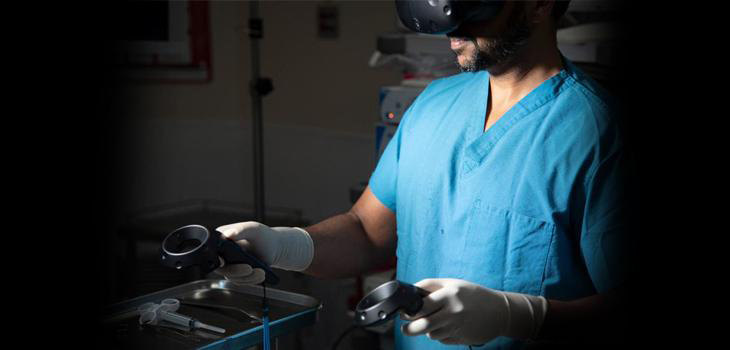 One of the main issues with traditional orthopaedic training programs is that they’re unable to keep up with the rapid introduction of new technologies, making them rather inefficient. There’s also a cost burden too.
One of the main issues with traditional orthopaedic training programs is that they’re unable to keep up with the rapid introduction of new technologies, making them rather inefficient. There’s also a cost burden too.
Precision OS use VR technology to complement existing bioskills training, address the gaps created by fractionated exposure and combine contextual learning and technical skills acquisition. Their technology is also used by practicing surgeons to maintain and upgrade their skills.
Precision OS offer tailored training modules designed around structured purposeful practice and productive failure. Their competency-based training reduces training hours and improves competency by efficiently combining knowledge and technical skill acquisition.
The technology replicates surgical workflows authentically, recreating physical environments and variable patient pathologies to provide real-life experiences that advance and internalize learning.

Like Precision OS, Fundamental VR also provide a cutting-edge VR technology that’s changed the face of medical education.
This is one of the leading medical education platforms for delivering multimodal simulation and education across tethered and all-in-one VR, mixed reality and mobile using AI. In partnership with innovative data infrastructure companies like 5G and Edge, FundamentalVR are ready to push the boundaries of immersive experiences.
The same goes for the exciting Californian-based, Osso VR, who use VR to provide content, tools and a platform to bridge the surgical training gap.
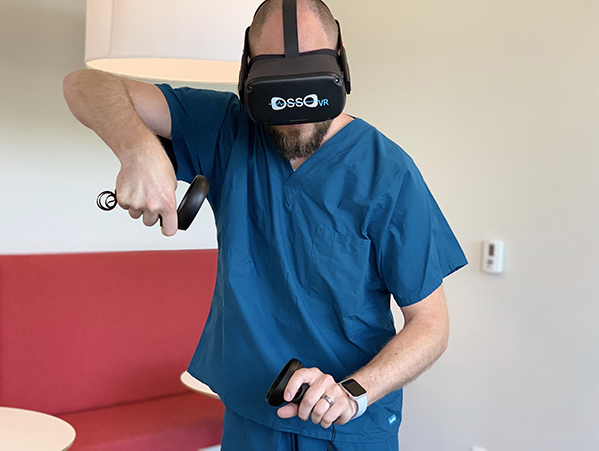
Their mission is to improve patient outcomes, increase the adoption of higher-value medical technologies and democratize access to surgical education around the globe. Osso VR work with many of the world’s top orthopaedic hospitals and device companies.
These companies have proven the value of innovation. In their own way, each technology is improving patient care around the world.
VR is connecting the global orthopaedics community, giving access to training on the latest devices and facilitating collaboration between experts. This is leading to more efficient training programs and higher skilled surgeons, freeing-up time to address the patient backlog. Meanwhile, POV and RPM devices are uniting surgeons and physicians with patients to provide more attentive care and limit the risk of infection from COVID-19.
If you'd like to chat about this article, any of the technology involved or want to tell me about something I’ve missed, please get in touch at Lloyd.Hines@medical-cm.com. I am also available to talk about servicing your recruitment needs.
Recommended.
Innovative Spine & Orthopedic Implant Technologies to Watch.
Orthopedics isn’t necessarily a market commended for its digital innovation, but these five companies are proving differently with their latest product launches. Click to read more.
What Innovations Could Shape the Future of Orthopaedics?
To achieve personalised care in orthopaedics, we need advances in AI, surgical robotics, augmented reality (AR) and more! But where will this innovation come from? Click to find out.
3 Technologies Revolutionising Spinal Surgery.
New innovations have continued to advance surgery – especially within the spinal space. I wanted to highlight the revolutionary technology that is driving this change and shaping the future of the space.

How to Take Your Medical Device to Market.
In this episode, I'm joined by Steven Haken and Deborah Rizzi from market access and reimbursement specialists Odelle Technology to discuss how to take a medical device to market.
Comments.